America’s #1 Killer Has New Foes
FIU researchers drive early detection and innovative cardiovascular care
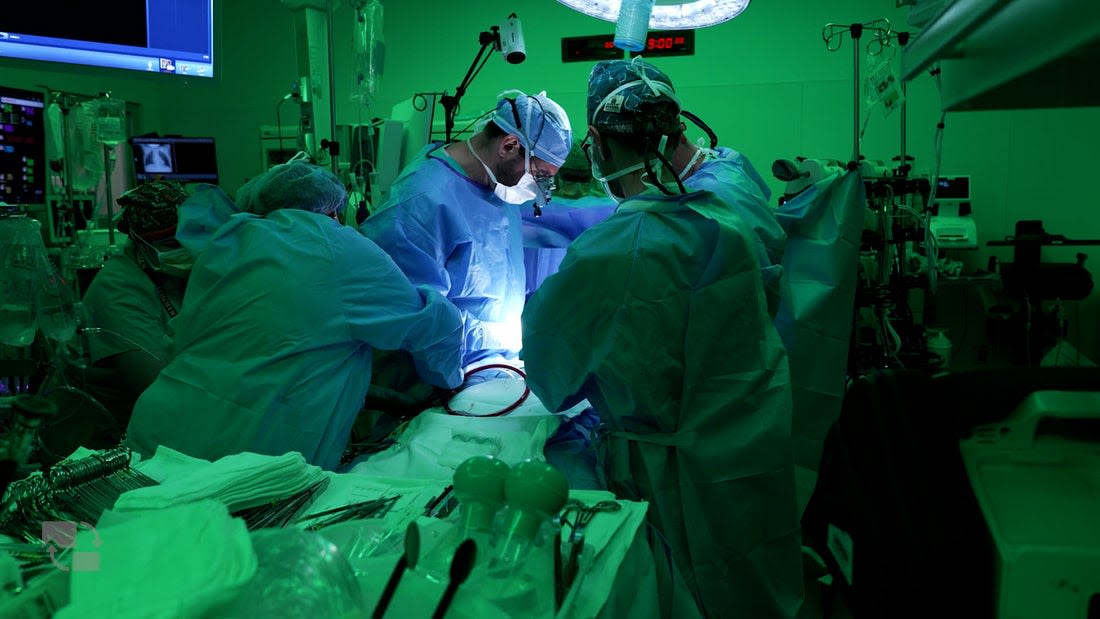
Cardiovascular disease has been the nation’s leading cause of death for over a century. The American Heart Association estimates at least six in 10 U.S. adults (more than 184 million people) will have some type of cardiovascular disease by 2050.
At Florida International University (FIU) and beyond, researchers, physician-scientists and cardiac surgeons focus their life’s work around addressing this problem. In their labs and the clinic, they are leading major technological and life-saving therapeutic advances to gain a deeper understanding of how cardiovascular disease happens and transform how it is prevented, detected and treated.
HEARING HEART DISEASE
“Heart disease doesn’t have a single solution,” said Joshua Hutcheson, an American Heart Association Fellow and director of the FIU-Florida Heart Research Foundation Center for Innovation in Cardiovascular Health. “But when you bring together people with different expertise and a shared purpose, real breakthroughs happen.”
Hutcheson and researchers in his Cardiovascular Matrix Remodeling Lab use cutting-edge engineering approaches to identify potential therapeutic targets and create new tools to detect cardiovascular disease in asymptomatic patients.
Working with Research Assistant Professor Valentina Dargam, he developed an AI-based algorithm that analyzes heart sounds and can identify disease signatures that are too subtle for the human ear. The AI-based diagnostic algorithm is 95% accurate in classifying healthy heart sounds and nearly 85% accurate in differentiating between types of heart disease. It also picks up on disease before cardiac murmurs or structural changes appear.
Dargam and Hutcheson will work with Dr. Tom C. Nguyen — chief medical executive of Baptist Health Heart & Vascular Care, as well as chair and professor in the Department of Cardiovascular Sciences at the FIU Herbert Wertheim College of Medicine — to test the technology in the clinic.
“This type of work is critical and the only way to advance medicine,” Nguyen says. “Physicians interact with patients on a daily basis and have a deep understanding of the clinical side of medicine. The team at FIU has a very strong foundation of cardiovascular research. Bringing the two together is a perfect marriage where we all complement each other.”
Joshua Hutcheson
Joshua Hutcheson
“Heart disease doesn’t have a single solution”
Valentina Dargam
Valentina Dargam
ROBOT IN THE OR
Relevant research that addresses real-world medical needs is at the heart of FIU’s strategic partnerships with Nicklaus Children’s Health System and Baptist Health South Florida. These collaborations have attracted world-renowned talent, including Dr. Makoto Hashimoto, an internationally acclaimed cardiac surgeon pioneering new approaches to robotic-assisted cardiac procedures.
Dr. Makoto Hashimoto
Dr. Makoto Hashimoto
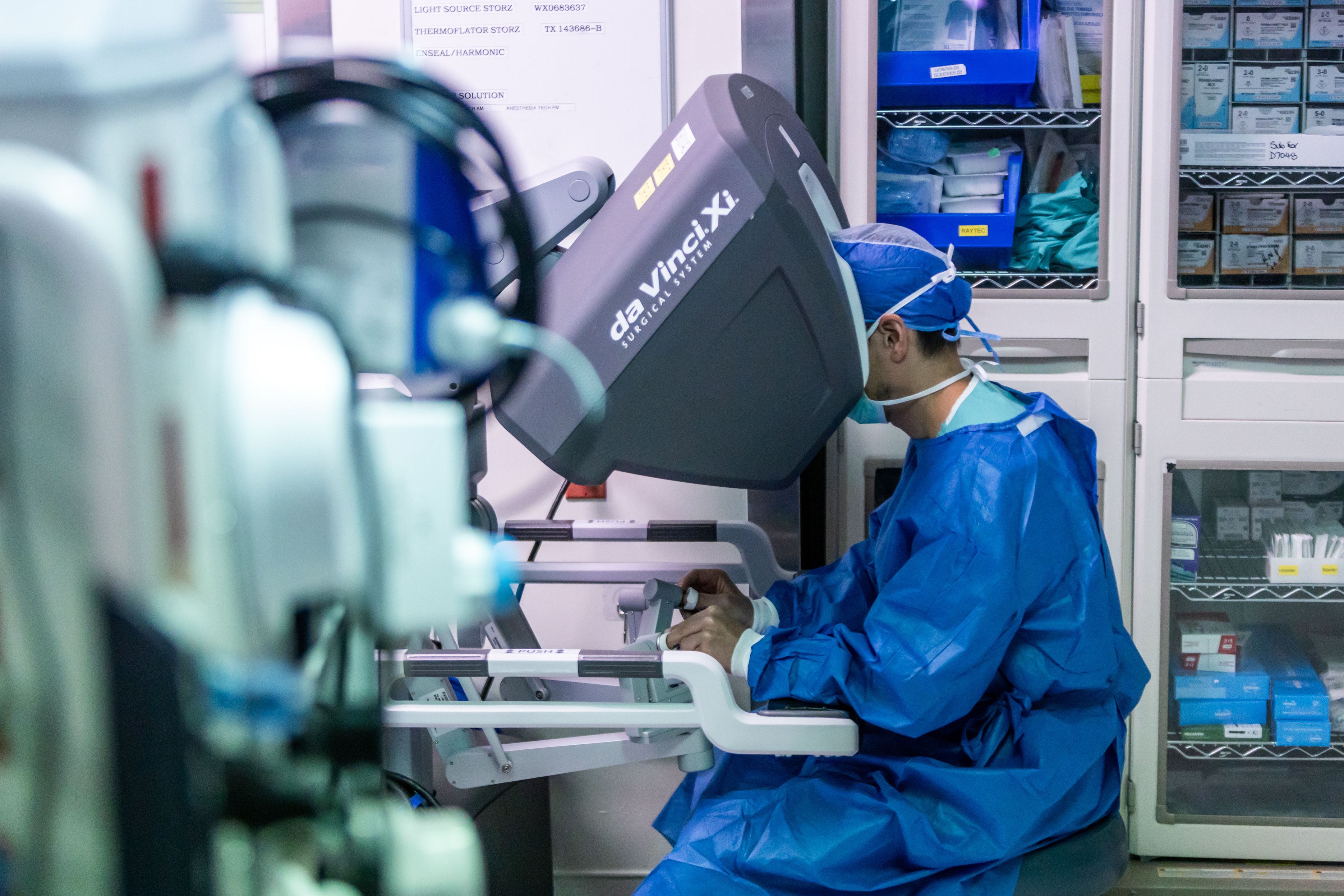
“The robot becomes part of my body during surgery,” said Hashimoto, FIU professor and director of robotic cardiac surgery who treats patients at Baptist Health Miami Cardiac & Vascular Institute. “It feels like an extension of myself.”
Because robotic surgery has many advantages — less pain, minimal scarring, faster recovery — it’s becoming increasingly popular with patients. But widespread adoption is lagging behind other specialties. Few cardiac surgeons perform more than 20 robotic cases a year. Hashimoto, however, performs hundreds. With an ever-growing volume of cases, he’s leading Florida’s busiest and fastest-growing robotic cardiac surgery program.
Every surgery Hashimoto completes saves another life. It also helps move the field forward by providing much-needed evidence that demonstrates novel robotic techniques can be applied safely and effectively to various conditions that once required more invasive procedures.
FIU medical student Natasha Mazinani, one of Hashimoto’s mentees, is helping advance this important work. She’s helped Hashimoto with case studies on complex conditions. One detailed how Hashimoto repaired a heart defect involving both a hole between heart chambers and a leaking valve (known as an atrioventricular septal defect with severe mitral regurgitation).
“I am so grateful to play a small role in advancing what we know about robotic procedures, because it’s a whole new realm,” Mazinani said. “It makes me really excited as a future physician about what advancements are yet to come.”
SAVING BABIES WITH HEART DEFECTS
For the estimated 40,000 children born with congenital heart defects, FIU physician-scientist Dr. David Kalfa is pushing the boundaries of what is surgically possible.
“We still don’t have many good options in terms of heart valve replacement for children with congenital heart defects,” said Kalfa, chief of cardiovascular surgery and co-director of the Nicklaus Children’s Heart Institute, as well as professor in FIU’s departments of pediatrics and surgical sciences. “The options we do have either aren’t small enough or can’t grow with the baby or child. Each time we need to replace it, that’s another open heart surgery.”
Living allogenic valve transplantation (also called partial heart transplants) has emerged as a promising alternative. Because even if heart muscle is damaged or diseased, the valves can be in good working condition.
In 2023, Kalfa performed the world’s first domino infant partial heart transplant while at New York-Presbyterian Morgan Stanley Children’s Hospital: An 8-month-old received a full heart transplant, and the healthy valves from her old heart were donated to a 2-month-old baby.
As with many things in life, logistics and timing have to align for partial heart transplants to be a success. That’s why Kalfa’s team is on a mission to extend the extracorporeal time of this precious tissue. He and his FIU research team are developing a bioreactor system that allows donated heart valves to be preserved for weeks — effectively “banking” tissue. This approach could provide the first off-the-shelf living valve replacements that grow with children, addressing the critical need for cardiac valves capable of growth and self-repair in pediatric patients with congenital valve disease.

This content was paid for and created by Florida International University. The editorial staff of The Chronicle had no role in its preparation. Find out more about paid content.







